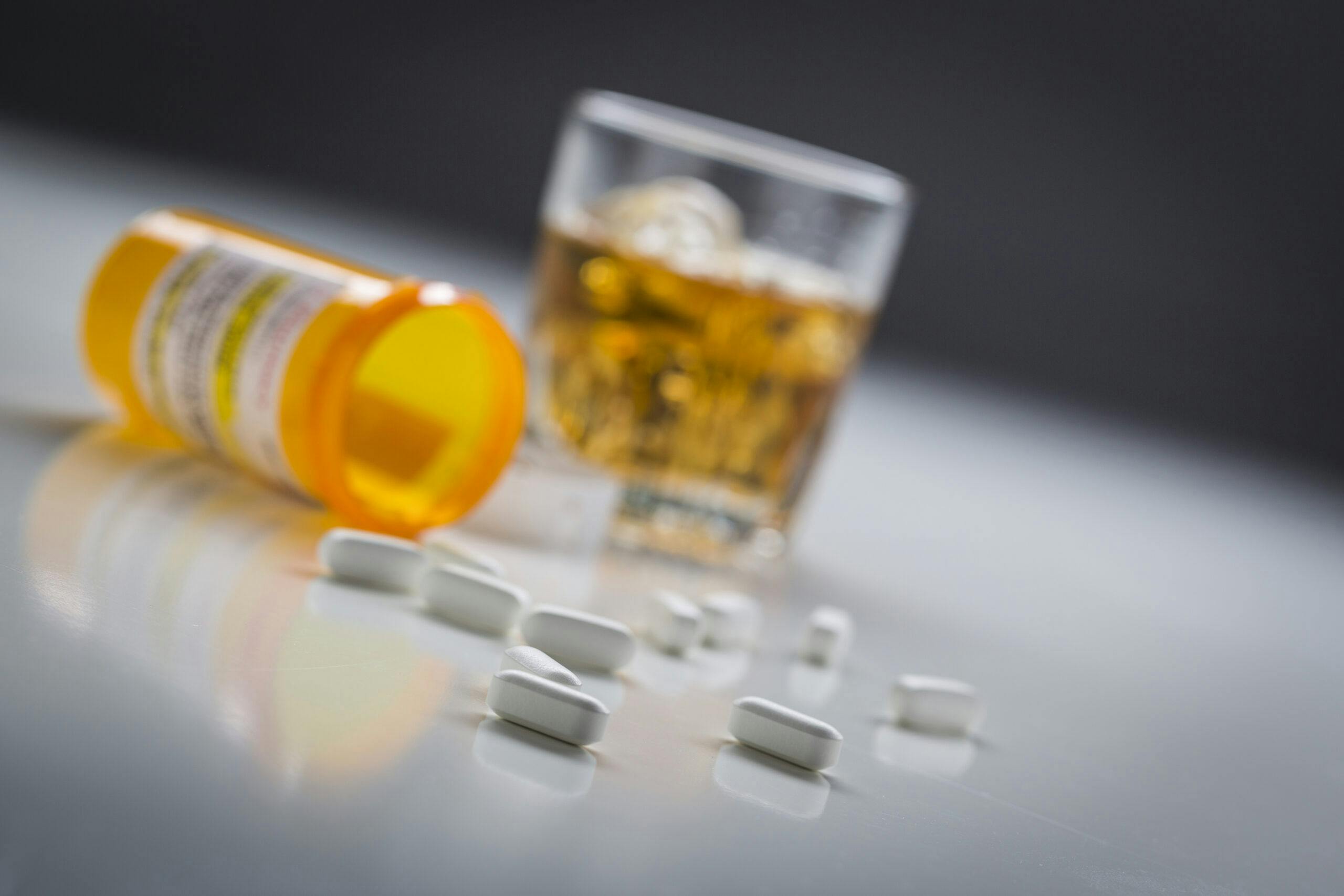
What Are The Dangers of Mixing Alcohol With Xanax?
Xanax (alprazolam) is used to treat muscle spasms, anxiety, seizures, and insomnia. Mixing Xanax with alcohol increases the risk of impaired judgment and overdose.
The active ingredient in Xanax produces a calming effect by enhancing the effects of GABA, an inhibitory neurotransmitter that naturally blocks and controls impulses in the central nervous system. However, combining benzodiazepines with alcohol can be dangerous and even deadly.
Are you or a loved one you know taking Xanax with alcohol? Overcoming a substance use disorder (SUD) can be challenging, and even more so when it involves two substances. Zinnia Health offers addiction treatment programs for co-occurring disorders. For more information, reach out online or call (855) 430-9439 today — we’re available 24/7.

What Are The Dangers of Mixing Xanax With Alcohol?
Xanax (alprazolam) is a prescription drug used by individuals who suffer from anxiety, insomnia, and seizures. Mixing Xanax and alcohol can make you feel more drowsy and intoxicated, as well as cause the side effects of Xanax to be worse.
The low-dose relaxing effect is what most recreational users strive for, but increased substance tolerance over time or accidentally taking too much can put a person at risk of more severe side effects.
As the amount of either substance increases, a person will begin feeling stronger behavioral inhibitions caused by the drug. Those inhibitions can cause poor coordination, clouded thinking, lethargy, and even a loss of consciousness. At high rates, Xanax and alcohol begin to suppress vital functions, including breathing and heart rate. This dangerous combination can also lead to behavioral inhibitions and an increased risk of overdose.
Can You Drink on Xanax?
No, when your doctor prescribes Xanax (alprazolam), you should not drink any alcohol. Alcohol can alter how the drug works in your body, putting you at a greater risk of dangerous activities, side effects, overdose, and even death.
How Long After Taking Xanax Can You Drink Alcohol?
After taking your last dose of Xanax, you should wait for a minimum of 48 hours (or longer if you fall within certain groups) before considering drinking alcohol.
The mean half-life of Xanax in healthy adults is 11.2 hours. Most drugs require four to five half-lives to be completely eliminated from the body. This means it will take 45-56 hours (about 2 days) before Xanax is out of your system. However, for certain populations, it may take about 3 to 4 days or longer for Xanax to be eliminated due to higher half-lives: healthy older adults (16.3 hours), people with alcoholic liver disease (19.7 hours), and the obese (21.8 hours).
Why Do People Mix Alcohol With Xanax?
Some people will choose to combine Xanax with other substances, such as alcohol. People with problems drinking alcohol have a higher rate of Xanax misuse. The goal of combining drugs is to enhance the effects of one or both substances. In the case of Xanax, combining it means achieving intense euphoria, an elevated sense of well-being, and even a sense of giddiness. The specific combination of Xanax and alcohol poses a number of risks.
Why Is It Dangerous to Mix Xanax with Alcohol?
On its own, alcohol is a central nervous system depressant (CNS), much like Xanax. Both Xanax and alcohol reduce neuron firing in the central nervous system, leading to a host of side effects. The exact outcome of the Xanax and alcohol combination depends on how much of each a person takes.
Combining Xanax with alcohol is dangerous. Alcohol is a depressant that also affects the brain and central nervous system, which is why it has a calming, sedating effect. In addition, alcohol often enhances the effects of prescription medications, which can lead to more inhibition. Also, alcohol often makes other drugs less effective, further increasing the chance of addiction and Xanax overdose.
What Can Happen if You Drink on Xanax?
Mixing Xanax and alcohol together can lead to some or all of the following complications:
1. Risk of Dangerous or Fatal Activities
The combination enhances the effects of both drugs, leading to a greater risk of dangerous or fatal activities such as impaired motor skills and cognition for driving. A person combining these drugs will experience severely impaired judgment and memory. They may forget how much they have been taking and continue to take more.
2. Increased Risk of Overdose
Xanax is potent on its own, but when it is mixed with alcohol, the risk of overdose greatly increases — 1 in 5 benzo-related deaths was due to alcohol. That’s because problem drinkers tend to increase doses.
However, a person can suffer a serious overdose even with a small amount of Xanax if they’re mixing it with alcohol. The reason is both drugs work together with the same mechanism of action, affecting the body in the same way with amplified sensations.
3. Longer Xanax Retention
When a person mixes Xanax and alcohol, their system is faced with a major burden. It becomes much harder for their system to process both, and it takes longer for the drugs to exit the system completely. This leads to individuals retaining more Xanax than they typically would because the liver must metabolize the alcohol before it can metabolize the Xanax.
4. Cognition Is Impacted
Combining alcohol and Xanax can have long-term effects that impact cognition and cause permanent issues with memory, attention, and problem-solving, as well as other mental processes. Long-term use can also result in physical side effects, such as liver damage, kidney damage, and cardiovascular system impairment, among others.
Combining alcohol and Xanax is sure to lead to dependence after multiple uses. Unfortunately, untangling the severe withdrawal symptoms that this drug combination can induce isn’t easy. Understanding those withdrawal symptoms and the detox process as a whole is an important step in getting help.
It’s vital to avoid the negative, and sometimes deadly, consequences of mixing Xanax with alcohol. If you have Xanax addiction and alcohol addiction, the team of treatment providers at Zinnia Health can help you get on the road to recovery. Reach out to speak with a rehab specialist today and learn about our detox and rehab programs.
What Are the Symptoms From Drinking Alcohol with Xanax?
Both alcohol and Xanax have a high misuse potential. Using alcohol and Xanax together regularly represents rapid habit formation and rapid tolerance development. This means dependence is sure to form over time.
Drug dependence is marked by altered body chemistry, where the body has grown so accustomed to having the drug in its system that it does not function properly without it. This means when someone stops taking Xanax, alcohol, or any other drug they’ve become dependent on, they can experience a range of negative side effects.
The negative side effects associated with reducing or stopping a drug are known as withdrawal symptoms. Withdrawal symptoms for Xanax can set in within hours of the last dose, and they can be serious.
Not only are withdrawal symptoms uncomfortable, but they can also prove life-threatening. That’s why stopping “cold turkey” or suddenly quitting Xanax is not recommended. Instead, you’ll need to work with a medical professional to gradually taper back your dosage.
Withdrawal symptoms will last for the entire period of the detox process. The detox period is however long it takes your body to get the drugs completely out of your system and restore itself back to its normal state.
The physical symptoms of withdrawal begin with the following:
- Headaches
- Blurry vision
- Numb fingers
- Sweating
- Anxiety
- Panic disorder
- Paranoia
- Insomnia
- Muscle pain
- Tremors
- Diarrhea
- Sensitivity to light/sound
- Loss of appetite
- Heart palpitations
Typically, the physical symptoms of withdrawal peak within the first four days of detox, but that doesn’t mean the symptoms are gone. T
he psychological symptoms of withdrawal can continue for weeks after your last dose, which is why entering a rehabilitation program is essential for ensuring that a person does not relapse.
Most often, the long-lasting symptoms of withdrawal include:
- Anxiety
- Insomnia
- Irritability
- Agitation
- Drug cravings
Benzodiazepines are among the most prescribed of any drug class in the United States thanks to their many uses. The medical use of Xanax is highly controlled, with the drug given in small doses, for short periods of time, and then tapered off gradually.
Xanax use can easily lead to drug abuse and drug addiction. Unfortunately, misusing Xanax poses great risks, especially since people tend to mix Xanax with alcohol or stimulants.
How to Get Help for a Xanax Addiction
Whether a person is using Xanax on its own or in combination with other drugs, such as alcohol, it’s essential that they enter into a proper treatment program. That’s because the symptoms of alcohol, along with the enhanced effects of Xanax, can lead to dangerous behavior, long-term effects, and overdose.
The first step of any treatment program is a thorough assessment of the individual. During the assessment, a medical professional will determine their condition and form a personalized pathway to help them safely and permanently recover.
1. Assessment
Misuse of any drug can lead to dependence. Once dependence forms, quitting on your own is simply not possible. Dependence leads to the onset of severe withdrawal symptoms that are uncomfortable and even life-threatening. Upon admission, medical intervention is often necessary for recovery.
If a person is using Xanax in combination with another substance, they’ll be diagnosed with a polydrug disorder. If that substance is alcohol, their medical professional will talk to them about alcohol use disorder. It’s possible for someone to be taking two or more drugs together and only have a dependence on one of them.
The types, amounts, and frequency at which you have taken certain drugs will impact the detox timeline and what therapies are used to help manage your withdrawal symptoms.
2. Detox Process
As soon as a person finishes the admissions process, they’ll enter the detox period. For an inpatient treatment facility, the detox process is fully managed with medical supervision and possibly medications to help reduce withdrawal symptoms.
Other therapies, such as talk therapy and wellness classes, may also be available. For a partial hospitalization or outpatient care plan, the detox process may involve take-home medications and multiple weekly meetings.
How long the detox process lasts depends entirely on the individual. No two recovery plans are alike. Every individual is treated based on their unique circumstances, needs, and goals, which means the timeline varies from one person to the next.
In general, withdrawal symptoms for Xanax peak within four days, and the hardest part is over within one to two weeks.
3. Rehabilitation
Once a person progresses from detox, they enter the rehabilitation phase. This phase can take some weeks or months to complete and is unique to the individual. Rehabilitation typically involves a combination of therapies, including talk therapy, peer support groups, wellness classes, nutrition classes, and more.
Inpatient residential rehabilitation is the most involved option and requires residing at a treatment center full-time. A person will meet with care staff daily and interact with other residents. Activities are often planned, and other amenities are available, including fitness centers and movie theaters.
For partial hospitalization and outpatient rehabilitation, individuals reside in their own homes but visit a treatment center or meeting place multiple times a week. Partial hospitalization is more intensive than outpatient rehabilitation and may involve daily meetings.
4. Continuing Care
When structured rehabilitation ends, an individual begins to transition back to normal life as they enter the aftercare period. At Zinnia Health, we are firm believers that a strong support system and ongoing discussions are essential to permanent recovery and avoiding relapse. That’s why we continue to offer the same level of personalized care long after an individual completes structured treatment.
Are you interested in learning more about how Zinnia Health approaches substance abuse and mental health treatments for Xanax abuse, alcohol abuse, and other addictions? If you or a loved one take Xanax and alcohol, it’s important to seek help. Contact our team today to explore your treatment options and take the first step.
Related Articles